Diabetes mellitus is a chronic metabolic disorder that results in increased blood sugar levels beyond normal (a fasting blood sugar level of 99 mg/dL or lower is normal). During digestion, food is metabolized into sugars and released into the blood. Insulin released from pancreatic cells helps transportation of these sugars to body cells for conversion into energy. When insulin production is insufficient or body cells do not respond to insulin, blood sugar levels rise above normal values. These high sugar levels will have ill effects on multiple organs in the body.

There are 3 types of diabetes: Type 1, Type 2, Gestational diabetes
This is commonly seen in children and young adults due to insufficient production of insulin.
This is the most common type of diabetes. Seen in adults over 45 years of age. This is due to the poor response of body cells to insulin signals. Insulin production is normal in the body but its utilization is abnormal.
Is commonly seen during pregnancy and becomes normal after delivery of the child.
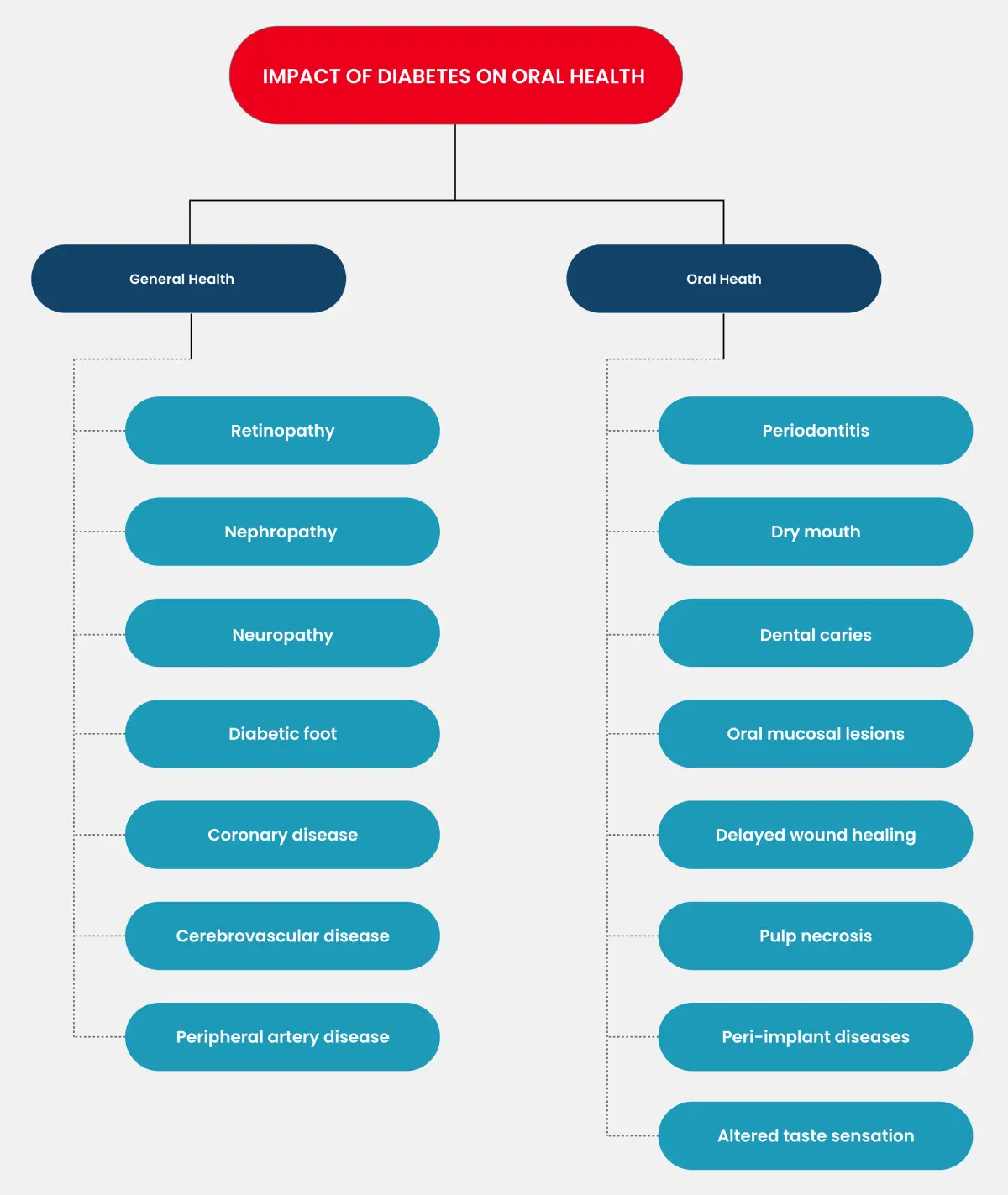
Diabetes mellitus affects the cardiovascular, renal, optical and neuromuscular. Along with general health diabetes also causes severe oral problems.
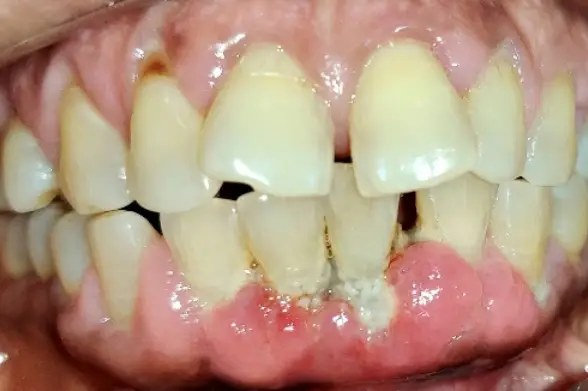
Periodontitis is the destruction of supporting tissues of teeth that involves periodontal ligament, bone and gingiva. Periodontitis is considered as the sixth complication of diabetes. Uncontrolled diabetes results in severe gum and periodontal diseases due to defective defence mechanisms (defective neutrophil activity) and degenerative changes in the periodontal ligament.
Reduced saliva production known as hypo-salivation or xerostomia is one of the most common problems seen in diabetes mellitus patients. Hyposalivation or xerostomia is more severe in patients with poorly controlled diabetes than in controlled diabetes. The reason behind the hyposalivation was unclear. Few studies show that diabetic neuropathy is reason for impaired function of salivary glands. Few histological studies showed that it is due to the degeneration of salivary gland cells.
Incidents of dental caries are high in diabetes, especially uncontrolled diabetes. Saliva protects the teeth by neutralizing the acid produced by Carlo genie bacteria. Hyposalivation and altered salivary composition in DM patients increases the risk of dental caries.
Dry mouth and defective immune system in uncontrolled diabetes increases the incidence of oral candidiasis infection. Fissured tongue, oral ulcers and burning mouth are other common findings noticed in diabetes.
Structural changes in collagen and defective immune system in diabetes results in delayed wound healing in diabetes patients. It takes a long time for the healing of extraction sockets and other oral lesions in DM patients, especially in uncontrolled DM. Osseointegration in implants procedure also affected in uncontrolled DM.
Diabetic patients usually have altered or decreased taste sensation compared to non-diabetics. Sensory nerve Neuropathy or dry mouth could be the reason for this complaint.
In controlled diabetes accumulation of glycation end products in the pulp tissue of teeth leads to structural changes and inflammatory reactions leading to pulp necrosis. These cases require Root Canal Treatment.
Incidents of peri-implant disease is high in patients with uncontrolled diabetes in whom missing teeth are replaced with implants. Peri implant mucous affects the soft tissue around the implant and peri-implant affects the bone around the implant. This will decrease the stability of the implant and leads to failure.